The Loneliest Generation: Inside Gen Z's Mental Health Crisis
Gen Z is the most diagnosed, most therapy-utilizing, and most openly distressed generation ever recorded — and the systems meant to support them are failing at nearly every level.
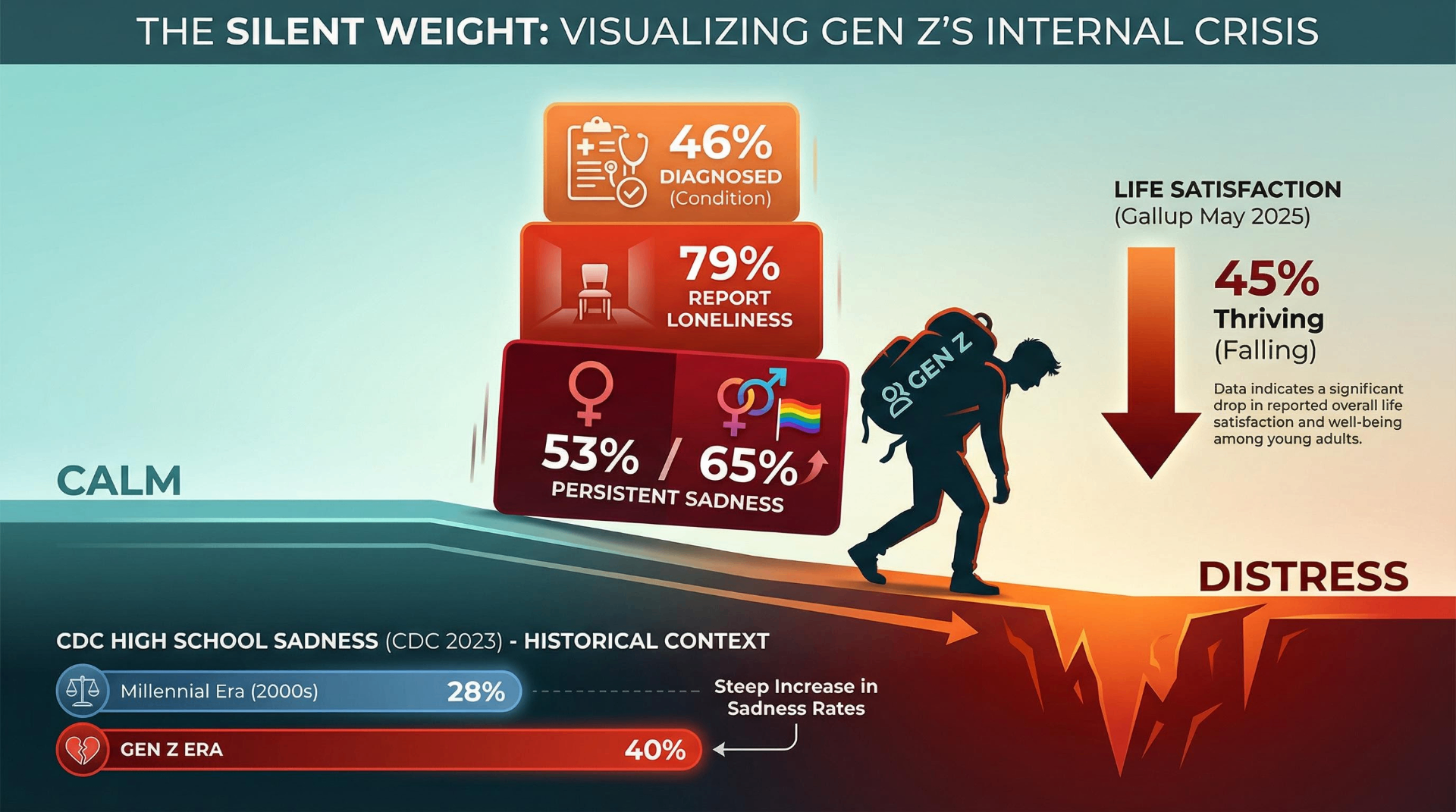
Gen Z is the most diagnosed, most therapy-utilizing, and most openly distressed generation ever recorded — and the systems meant to support them are failing at nearly every level. Roughly 46% of Gen Z Americans have been diagnosed with a mental health condition, their life satisfaction is falling (only 45% are "thriving" per Gallup's May 2025 data, down from 49% a year earlier), and up to 79% report experiencing loneliness. These numbers represent more than a statistical anomaly or a generational tendency toward complaint. They reflect a genuine structural crisis shaped by the collision of algorithmic technology, economic precarity, institutional decay, and a radically altered developmental environment — all unfolding against the backdrop of pandemic disruption, climate dread, and the erosion of community life that sociologists have tracked for decades. What follows is a synthesis of the best available evidence (2022–2026) across five dimensions: technology, systemic failure, identity and coping culture, generational comparison, and class — aimed at understanding not just what is happening, but why, and for whom it is worst.
A generation in crisis, by the numbers
The data converge from every major research institution. The CDC's 2023 Youth Risk Behavior Survey — the most recent available, released August 2024 — found 40% of high school students reported persistent feelings of sadness or hopelessness, with 20% seriously considering suicide and 9.5% attempting it in the past year. These figures represent a modest improvement from the 2021 post-pandemic peak (42% and 24%, respectively for sadness and serious suicidal ideation among girls), but remain dramatically elevated compared to the early 2000s, when roughly 28% of Millennial-era high schoolers reported comparable distress.
The gender gap is stark and widening. 53% of female students reported persistent sadness or hopelessness in 2023, and 27% seriously considered suicide. LGBTQ+ students face the most acute crisis: 65% experienced persistent sadness, 41% seriously considered suicide, and 20% attempted it. Among racial groups, Black youth suicide rates have surged 37% between 2018 and 2021, the largest increase of any demographic, and for the first time in 2024 provisional data, Black young adults aged 20–24 surpassed white peers in suicide rates.
SAMHSA's 2024 National Survey on Drug Use and Health, released in 2025, found 32.2% of young adults aged 18–25 experienced mental illness and 12.6% had serious thoughts of suicide. The APA's November 2025 Stress in America report — subtitled "A Crisis of Connection" — found 54% of Americans feel isolated and 50% lack companionship. Harvard's Spring 2025 Youth Poll found 42% of young Americans say they are "barely getting by" financially, only 17% report deep social connection, and only 15% believe the country is headed in the right direction.
One emerging bright spot: youth suicide mortality appears to have declined in 2024, according to a JED Foundation analysis of CDC data, driven primarily by reductions among boys and young men. Whether this represents a turning point or a temporary fluctuation remains unclear. Meanwhile, school violence indicators are moving in the wrong direction — students missing school due to safety concerns rose from 9% to 13% between 2021 and 2023, and bullying at school increased from 15% to 19%.
The great rewiring: screens, algorithms, and the causation war
No dimension of this crisis generates more heat than the role of smartphones and social media. The debate has intensified since Surgeon General Vivek Murthy issued his May 2023 advisory declaring social media a "major threat" to youth mental health, noting that teens spending more than three hours daily on social media face double the risk of depression and anxiety symptoms. In June 2024, Murthy escalated to calling for congressionally mandated warning labels, comparing the platforms to cigarettes. Forty-two state attorneys general endorsed this call, and New York State passed legislation in 2025 requiring warning labels on platforms with addictive design features for users under 18.
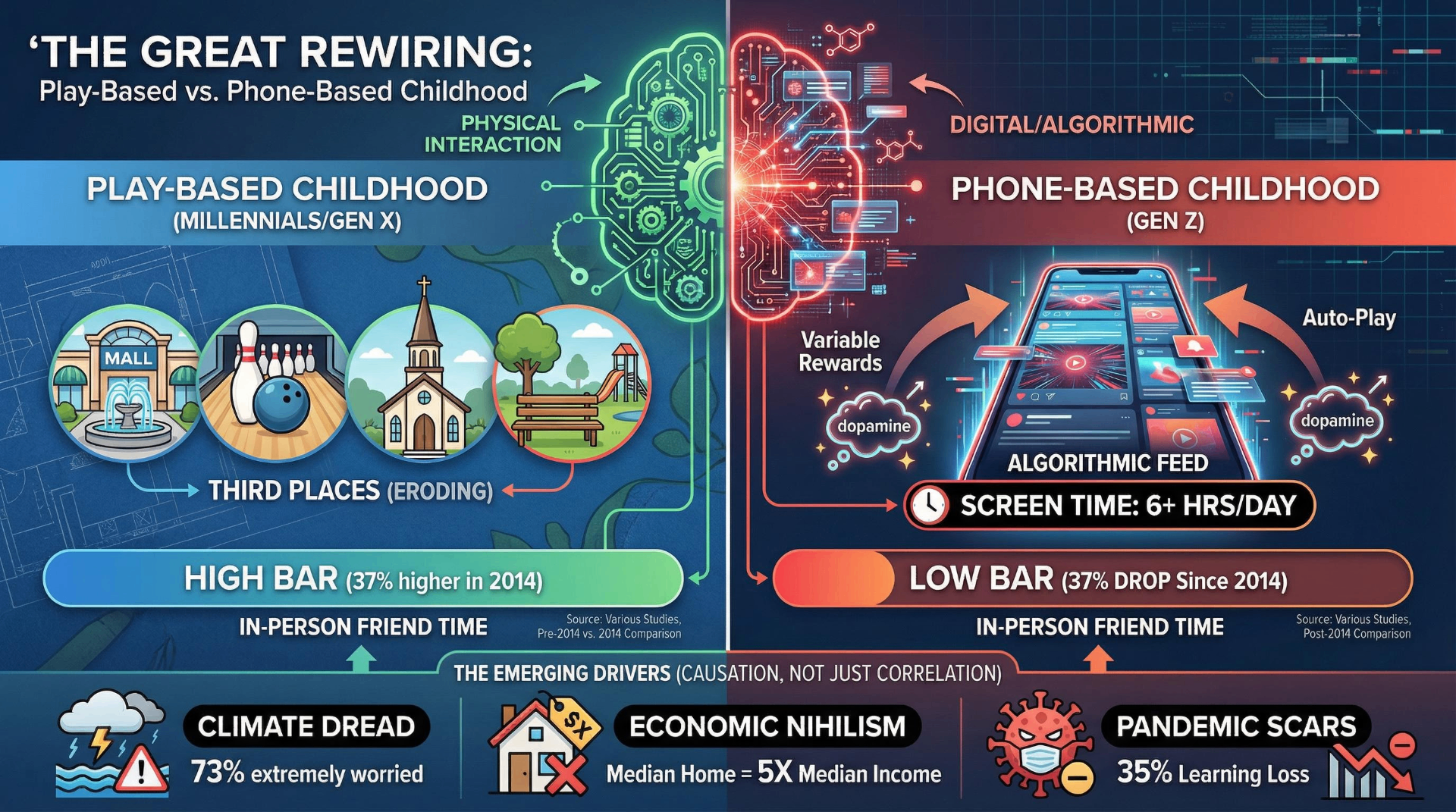
Jonathan Haidt's The Anxious Generation (2024), which sold over two million copies and spent months atop bestseller lists, crystallized the technological thesis. Haidt argues that between 2010 and 2015, a "phone-based childhood" replaced a "play-based childhood," fundamentally rewiring adolescent development. His data points are striking: time Americans spent with friends dropped 37% between 2014 and 2019; Gen Z high school seniors spend roughly an hour less on in-person social interaction than early Millennials did; and the timing of the mental health decline aligns precisely with the mass adoption of smartphones with front-facing cameras and algorithmic social media feeds.
The neuroscience offers some support. A 2025 review in PMC examining 40 neurophysiological studies found frequent social media engagement alters dopamine pathways, with decreased gray matter density in the prefrontal cortex of heavy users. Platform design deliberately exploits these vulnerabilities: variable reward schedules (the unpredictable delivery of likes and comments), infinite scroll mechanisms that eliminate natural stopping cues, and auto-play features that trigger dopamine release through anticipation rather than satisfaction. A 2024 meta-analysis of nine prospective cohort studies found baseline screen time significantly predicted future depression (OR = 1.20), and a 2024 sleep study found two hours of LED tablet exposure caused a 55% decrease in melatonin production.
But the academic response to Haidt has been fierce and substantive. Candice Odgers of UC Irvine published a widely cited Nature review arguing his claims are "not supported by science" and risk distracting from the real causes of the crisis. Andrew Przybylski of Oxford criticized Haidt's methodology as "vote counting" — prioritizing the quantity of supporting studies over their quality. One analyst found that of the 476 studies Haidt cited, only 22 contain data on either heavy social media use or serious mental health issues among adolescents, and none examine both simultaneously. The most rigorous meta-analyses consistently find small average effect sizes — comparable, as Orben and Przybylski noted in their influential 2019 analysis, to the effect of wearing glasses or eating potatoes.
The most significant empirical test came from the SMART Schools Study, published in The Lancet Regional Health – Europe in February 2025. This first rigorous UK evaluation of phone-restrictive policies across 30 schools and 1,227 adolescents found no significant impact on mental wellbeing from restrictive phone policies — primarily because total screen time and social media use were unchanged outside school hours. A broader 2024 scoping review of 22 studies across 12 countries declared "inconclusive evidence" for phone ban mandates, though low-achieving, low-SES students showed the strongest academic benefits.
Where does academic consensus stand? There is broad agreement that a genuine mental health crisis exists among young people, and that social media use correlates with negative outcomes. The disagreement centers on causation, effect magnitude, and whether technology is the primary driver or one factor among many. The most sophisticated position may be that small average effects mask large effects on vulnerable subgroups — girls, LGBTQ+ youth, and those with pre-existing mental health conditions — while the broader population experiences more modest impacts. The causal question, given ethical constraints on experimental research, may never be definitively resolved.
Systemic fractures: from therapist deserts to unaffordable adulthood
If technology rewired the environment in which Gen Z develops, the systems theoretically designed to catch them — healthcare, education, economic opportunity — have simultaneously deteriorated. The United States faces a projected deficit of over 250,000 behavioral health practitioners across psychiatry, counseling, and social work. More than 115 million Americans live in federally designated mental health professional shortage areas. Rural communities are worst affected: some lack any licensed counselor within a 100-mile radius, while average wait times at community mental health centers have reached 73 days.
The insurance system functions as an additional barrier. More than a third of psychologists and 45% of psychiatrists do not accept insurance, driven by reimbursement rates averaging roughly $98 per session — far below the $200+ out-of-pocket rates that make private practice economically viable. An NPR/ProPublica investigation in 2024, interviewing over 500 therapists across nearly all 50 states, found insurers routinely determine the length and type of care, and more than a dozen therapists reported insurers urging them to reduce care even when patients were near suicide. The national average therapy cost hit $139 per session in 2024, up 13% in five years.
Policy developments in 2025 have moved in a troubling direction. The Biden-era mental health parity regulations, finalized in September 2024, would have required insurers to provide meaningful benefits and take corrective action when access disparities appeared in outcome data. In May 2025, the Trump administration announced it would not enforce these regulations. Proposed Medicaid cuts of $1 trillion over ten years threaten the single largest payer for mental health services in the United States.
The digital mental health boom has proved double-edged. Therapy apps expanded access — BetterHelp became the world's largest online therapy platform — but scandals revealed the costs. BetterHelp paid a $7.8 million FTC settlement in 2023 for sharing the health data of over seven million consumers with Facebook, Snapchat, and Pinterest for advertising. Cerebral paid $6.57 million to the DOJ for pressuring clinicians to overprescribe stimulants to boost patient retention. AI therapy chatbots like Woebot and Wysa show promise for mild-to-moderate symptoms, but a 2024 systematic review found their therapeutic effects are "small and not sustained over time," and only 16% of chatbot studies have undergone clinical efficacy testing.
In schools, the national student-to-counselor ratio sits at 372:1 — nearly 50% above the American School Counselor Association's recommended 250:1. Only four states meet the recommendation. About eight million children lack access to any counselor in their school. Schools that used federal pandemic relief funds to hire mental health staff now face losing those positions as ESSER funding expired in 2024, with counseling ranked among the top three spending categories.
Economic precarity compounds everything. Total U.S. student loan debt exceeds $1.7 trillion across 42.7 million borrowers. A 2024 Student Loan Planner survey of nearly 4,000 borrowers found 78.7% experienced anxiety, 41.5% depression, and 1 in 16 experienced suicidal ideation because of their loans — a figure that jumps to 1 in 8 for borrowers earning under $50,000. Housing is equally punishing: young adult renters under 25 are the most cost-burdened age group, with 60% spending more than 30% of income on housing. The stock of rental units below $1,000 per month dropped by over 30% in a single decade. A 2024 study of low-income Black young adults found those experiencing unaffordable or overcrowded housing were more than four times as likely to have depression compared to stably housed peers.
The pandemic left lasting developmental scars. A UC Merced study published in Scientific Reports in November 2024 found children tested post-lockdown showed significantly worse social cognition skills, with effects persisting into 2023, particularly for lower-SES children. A Gallup poll in February 2025 found 22% of parents say the pandemic's negative impact on their child's social skills is ongoing. A meta-analysis of 42 studies found children lost an average of 35% of a school year's learning — a loss that remained stable even after returning to in-person instruction.
Fluent in trauma: when mental health language reshapes identity
Gen Z's relationship to mental health is defined by a paradox: they are simultaneously the most emotionally literate generation in history and, by nearly every measure, the most distressed. An estimated 87% of Gen Zers feel comfortable talking about mental health. Forty-two percent are currently in therapy — a 22% increase since 2022. Three-quarters of Gen Z men say they would speak to someone about their mental health, a figure that would have been unthinkable for their grandfathers.
This openness has delivered real benefits. Destigmatization has enabled help-seeking at unprecedented rates, and Gen Z's willingness to name suffering has forced institutional change — from workplace mental health benefits (job descriptions mentioning mental health tripled between 2020 and 2024) to legislative action on social media. But the same cultural forces that reduce stigma also create new complications.
Therapeutic language has migrated from clinical settings into everyday discourse. Terms like "toxic," "triggered," "gaslit," "boundaries," and "attachment style" now function as social currency. Stanford professor Jamil Zaki warned in January 2026 that phrases like "protect your peace" can "morph into being selfish or a bad friend," providing sophisticated-sounding justification for social withdrawal at a moment when connection is what Gen Z most needs. Nick Haslam's influential "concept creep" framework documents how harm-related concepts — abuse, trauma, addiction, prejudice — have expanded both to encompass qualitatively new phenomena and to include less extreme variants of the original concept. Since the 1980s, there has been a "steep rise" in how harm language appears in English. The effect is ambivalent: broader concepts of mental disorder are associated with more favorable attitudes toward help-seeking, but they also risk pathologizing ordinary human distress.
The self-diagnosis phenomenon captures this tension precisely. Research from Harvard's Petrie-Flom Center found that 1 in 4 adults now suspect they have ADHD, while the actual prevalence is roughly 6%. A 2025 PlushCare analysis found 83.7% of TikTok mental health advice is misleading and 14.2% is potentially damaging. People are 5 to 11 times more likely to incorrectly self-diagnose than to correctly identify a mental illness. Yet the same platforms enable recognition of genuinely underdiagnosed conditions — particularly ADHD in women — and connect isolated individuals to communities that offer real validation and support.
"Performative wellness" represents the cultural endpoint of these dynamics. A 2023 Frontiers in Psychology study found that exposure to curated wellness content triggers upward social comparisons that predict lower self-esteem, even as surface-level self-esteem appears to rise — a suppression effect that captures the dissonance perfectly. As Psychology Today noted in 2025, "vulnerability has become aesthetic" — and the line between authentic emotional expression and performed emotional intelligence grows increasingly difficult to locate. A 2025 Frontiers comparative study demonstrated that adolescents show significantly more pronounced self-esteem fluctuations than adults in response to social media feedback, explained by neurodevelopmental models where the limbic system matures before the prefrontal cortex.
The deepest concern may be identity fusion — when a psychiatric diagnosis becomes a primary identity rather than a condition to be treated. The American Psychiatric Association's Focus journal warned in 2025 that "strongly identifying with a particular psychiatric diagnosis might interfere with treatment because making positive behavioral changes would thereby lead to the risk of losing a source of identity as well as a community associated with this identity." Writer Freya India has described how mental health diagnosis has moved "to the center of how a huge percentage of Gen Z young people define their whole beings." As a team of Boston College researchers framed it: "A generation steeped in mental health language — but still profoundly unwell."
Not your parents' adolescence: what's structurally different
The question of whether Gen Z's distress represents something genuinely new — or merely better-measured versions of perennial adolescent suffering — is central to every policy response. The evidence, on balance, supports the view that this crisis is substantially real, not merely artifactual, though measurement changes account for some of the increase.
The generational gradient is steep. A multi-year study found 65% of Gen Zers reported experiencing at least one mental health problem in the past two years, compared with 51% of Millennials, 29% of Gen Xers, and 14% of Boomers. A 2023 PNAS study using 20 years of Australian panel data found strong evidence that cohort effects — not just age or period effects — are driving mental health decline, concentrated specifically among those born in the 1990s. The trend appears simultaneously across multiple developed nations, suggesting common causes rather than local measurement artifacts. And objective indicators — suicide rates, emergency room visits for self-harm, psychiatric hospitalizations — have risen alongside self-report measures, weakening the argument that Gen Z simply reports more honestly.
Foulkes and Andrews's "prevalence inflation hypothesis" (2023) offers a partial counterargument: mental health awareness campaigns may lead some individuals to interpret normative distress as clinical pathology, inflating reported rates. A study comparing DSM editions found no overall change in diagnostic stringency across iterations, though specific conditions — particularly ADHD, autism, and eating disorders — showed evidence of diagnostic inflation. Cultural stigma almost certainly suppressed reporting in earlier generations: only 22% of Boomers have ever received therapy, and a 2024 study found Gen X maintains the highest mental health stigma scores across multiple measures.
But several structural features of Gen Z's environment have no historical precedent:
The phone-based childhood: Gen Z is the first generation to navigate puberty with smartphones and algorithmic social media. The 95% smartphone penetration rate, combined with an average of 6+ hours of daily screen time, represents an environmental exposure without analogue in prior generations.
Climate as existential threat: 73% of Gen Z globally report extreme worry about climate change, and over half believe "humanity is doomed." Close to 40% say climate fears make them reluctant to have children. No prior generation faced an equivalent consensus scientific warning about civilizational risk during their formative years.
The disappearance of third places: The community spaces where prior generations developed social skills — malls, arcades, bowling alleys, churches — have systematically eroded. Bowling leagues have declined roughly 95% over half a century. Religious participation among young women dropped from 29% to 19% between 2016 and 2024. Time with friends has been cut nearly in half.
Economic immobility as baseline expectation: The share of children earning more than their parents declined from roughly 90% for those born in 1940 to around 50% for those born in 1984, and has continued falling. Only 21% of 25–34-year-olds achieved all four traditional milestones of adulthood (living independently, working, married, with children) in 2024, down from 45% in 1975.
Intergenerational trauma transmission adds another layer. A 2024 study using data from over 54,000 adolescents found parental mental health significantly predicts adolescent outcomes, with maternal mental health having a stronger association with daughters and paternal with sons. Gen X parents — who navigated the 2008 recession during prime family-building years — transmit their own economic anxiety and attachment patterns to Gen Z children. Emerging epigenetic research, while still contested in humans, suggests trauma may alter gene expression across generations: Holocaust survivor descendants show distinct DNA methylation patterns associated with both heightened stress reactivity and enhanced social bonding.
Robert Putnam, whose Bowling Alone documented a half-century decline in social capital, stated at a 2024 Dartmouth symposium that his findings are "even more relevant now." His I-We-I framework tracks the arc from individualism around 1900 to peak community and equality in the 1950s–60s, then a steady return to isolation and polarization. Gen Z has inherited the lowest point of that curve, with social media offering a simulacrum of connection that research consistently shows fails to substitute for in-person community. Surgeon General Murthy's 2023 loneliness advisory cited Putnam extensively, declaring loneliness an epidemic with health effects equivalent to smoking 15 cigarettes daily.
The class fault line beneath the crisis
Perhaps the most underexamined dimension of the Gen Z mental health crisis is how sharply it stratifies by class. The data reveal not one crisis but two: an affluent version addressed by a $6.8 trillion global wellness industry growing at 7.6% annually, and a working-class version defined by therapist deserts, food insecurity, housing instability, and material deprivation that directly causes psychiatric illness.
The wellness economy's scale is staggering — four times larger than the global pharmaceutical industry, projected to reach $9.8 trillion by 2029. Its most visible manifestations serve the wealthy: $200,000 wellness club memberships, $69,000 psychedelic retreats, $250-per-session boutique Pilates. Per capita wellness spending in North America ($6,029) is thirteen times the rate in Asia ($471). McKinsey estimates 82% of U.S. consumers consider wellness a "top priority," but the industry is "doubling down on high-end consumers" while workplace wellness — the segment most accessible to average workers — actually shrank 1.5% in 2024.
At the other end, material deprivation functions as a direct psychiatric cause. Among low-income Black young adults, those experiencing housing instability were more than four times as likely to have depression and more than twice as likely to report anxiety. Twenty-three percent of undergraduates are food insecure — over four million students — and food-insecure students are 43% less likely to graduate. Suicide is the leading cause of death among youth experiencing homelessness.
The racial wealth gap compounds these disparities. Non-Hispanic white median household wealth stands at $187,300; for Black households it is $14,100 — a 13:1 ratio. Black borrowers hold 186% more student debt per capita than white borrowers and are more likely to attend predatory institutions. Among adults with fair or poor mental health, 50% of white adults received services versus 39% of Black and 36% of Hispanic adults. The mental health workforce is 86% non-Hispanic white, creating cultural barriers that research consistently identifies as deterrents to help-seeking.
The gig economy, in which roughly 43% of Gen Z workers participate, creates a new vector of precarity. Research published in Sage Journals found dependent platform workers — those solely reliant on gig income — report psychological distress levels comparable to unemployment, with financial strain explaining approximately half of the elevated distress. These workers lack health insurance, retirement benefits, and the social connections of a stable workplace, concentrating the most vulnerable demographics — young people, racial minorities, immigrants — in the least psychologically protective forms of labor.
Case and Deaton's "deaths of despair" framework, originally describing middle-aged white Americans dying from suicide, drug overdose, and alcoholic liver disease, is increasingly applicable to younger cohorts. Mortality from drug overdose and suicide among North American adults under 40 has increased by more than 40% since 2010. A 2025 study in Demography found that "cognitive despair" — hopelessness and pessimism — was the strongest predictor of mortality risk among young adults, associated not only with suicide and drug poisoning but even cardiovascular disease. Life expectancy for working-class Americans without a college degree peaked in 2010 and has declined since.
The emerging psychological concept of "financial nihilism" captures Gen Z's response to this landscape. When median home prices reach five times median household income, when the average 2022 graduate carried negative net worth of -$31,571, when only 9% of Gen Z adults own homes, the traditional narrative of economic participation — save, invest, plan — loses credibility. Fortune reported in January 2026 that Gen Zers experience "age and money dysmorphia," a persistent sense of falling behind, with short-lived coping mechanisms like "doom spending" functioning as psychological survival strategies rather than financial irresponsibility.

Where the evidence points, and what it demands
The Gen Z mental health crisis is real, multi-causal, class-stratified, and only partially responsive to the interventions currently available. The most honest synthesis of the evidence resists monocausal explanations. Social media and smartphones are neither the sole cause nor an innocent bystander — they are one powerful factor in a system that includes economic precarity, institutional failure, community erosion, climate dread, pandemic disruption, and the transformation of mental health language itself into a double-edged cultural force.
Three insights emerge from this research that deserve more attention than they typically receive. First, the crisis is not uniformly distributed: low-income Gen Zers, Gen Zers of color, LGBTQ+ youth, and those in rural areas experience it with far greater severity, and the solutions that reach them last are the ones they need most. A $6.8 trillion wellness industry that primarily serves the affluent while community mental health centers maintain 73-day wait lists is not a system working for its most vulnerable members.
Second, Gen Z's unprecedented openness about mental health has not, by itself, translated into better outcomes. The generation most fluent in therapeutic language is also the loneliest and most distressed — suggesting that awareness without access, vocabulary without community, and diagnosis without structural change are insufficient. The prevalence inflation hypothesis deserves serious consideration alongside the genuine crisis: both can be true simultaneously, and distinguishing between them matters for policy.
Third, the most promising interventions operate at the structural level rather than the individual one. Phone-free schools show academic benefits even when mental health effects remain unclear. Enforcing mental health parity in insurance would address the access gap that leaves 36.7% of young adults perceiving unmet need. Addressing housing affordability, student debt relief, and living wages would target the material deprivation that research now identifies as a direct psychiatric cause, not merely a "risk factor." The deaths of despair framework reminds us that when economic hopelessness becomes endemic, no amount of therapy — digital or otherwise — can substitute for a future worth believing in.
Gen Z is not fragile. They are the most help-seeking, most emotionally articulate, most willing-to-name-the-problem generation in recorded history. The question is whether the structures around them will prove worthy of that honesty — or whether they will continue to metabolize systemic failures as individual pathology, scrolling through feeds that promise connection while delivering comparison, in a world that offers them the language of healing but not always its substance.
Share Your Voice
Join the conversation to share your thoughts and help others understand this topic better.
Join the ConversationCommunity Feedback
No comments yet. Be the first to share your thoughts!